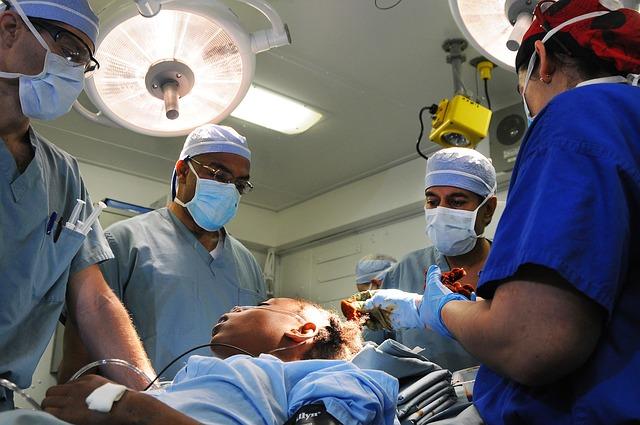
Photo credit: Pixabay, tpsdave
In medical school, America’s physicians receive a piece of advice that they rarely share with patients: “Don’t get sick in July.” To most Americans, who try to never get sick, it may seem like odd advice. But to doctors, especially those at one of the teaching hospitals that make up around one fifth of the country’s hospitals, it is a black humor joke.
Every July 1, newly graduated medical students begin their residencies, practicing medicine under the supervision of older physicians, while the most senior residents take on new roles as fully qualified physicians. In lockstep with the medical school calendar, the junior-level staffs at 20% of American hospitals are entirely disrupted. In some cases, individuals take on the role of the supervisor to whom they reported a day earlier.
As everyone adjusts to his or her new role, doctors make more mistakes and operate less efficiently. As surgeon Atul Gawande has written on the transition:
Residencies attempt to mitigate potential harm through supervision and graduated responsibility… But there is still no getting around those first few unsteady times a young physician tries to put in a central line, remove a breast cancer, or sew together two segments of colon. No matter how many protections we put in place, on average these cases go less well with the novice.
This comprehensive turnover at teaching hospitals — and its potentially deadly consequences — is not unique to the United States. Americans know this phenomenon as the “July Effect”; Britons know it as “the killing season.” The term was made famous by the television show Cardiac Arrest, in which a doctor consoles a young physician after he makes a deadly mistake: “You come out of medical school knowing bugger all. No wonder August is the killing season. We all kill a few patients while we’re learning.”
The July Effect: Urban Legend?
Cable news likes nothing more than an opportunity to warn people about a threat to their family’s well-being (“Coming up next, is your water bottle giving you cancer?”), so the absence of news spots on the July Effect is surprising. Given their awareness of the turnover, some doctors visiting a hospital for their own health care will ask a brand-new resident to go get his or her supervising physician. Where are all the exposés advising us to do the same?
One reason the public may remain relatively ignorant of the effect is that its consequences are hidden. Hospitals are most strained during winter months, when seasonal illnesses and weather lead to a surge in admissions, procedures, and fatalities. With the July transition fortuitously taking place during the calmer summer season, any resulting dysfunction can often seem no worse than the business of a January visit.
But the main reason is that doctors looking into the performance of teaching hospitals have been unable to find evidence of the July Effect. Medical journals regularly publish studies that look at data like the average length of stay in the hospital (an indicator of hospital efficiency) and a hospital’s mortality rate. They usually report finding no drop in the quality of care between July and other months at the teaching hospitals they investigate, or between teaching hospitals and regular hospitals in July and August.
One study, published in 2013, suggested that the July Effect was negligible for routine care, but very real in the case of high-risk procedures where even a slight delay can be deadly. The researchers’ evidence came from data on the treatment of high-risk heart attacks. It’s an intuitive conclusion, but also potentially belied by the number of studies that investigate complicated procedures like spinal surgery and appendicitis without finding any trace of July’s deadly legacy.
Reviewing the evidence, one ob/gyn resident advises graduating medical students that “the July phenomenon is most likely a myth.” The transition period may be stressful, but as long as interns are careful “not be the ‘n-value’ that adds to the body of evidence that provides validity to the July phenomenon in the year to come,” they’ll be fine.
It’s a comforting notion for patients as well. Unfortunately, it’s also contradicted by initial findings from another group of researchers.
The Ides of July
If your hospital stay was 2% longer, or your risk of death 4% higher, would that keep you away from the hospital in July? Or, if you had no choice in when you go, concern you?
As detailed in a working paper for the National Bureau for Economic Research, that is the estimated effect of the annual summer turnover in teaching hospitals. Unlike the aforementioned studies from the medical field, the paper, “Cohort Turnover and Productivity: The July Phenomenon in Teaching Hospitals,” is authored by Harvard Business School researchers, led by Professor Robert S. Huckman, interested in the impact of worker turnover on productivity.
Why would they find a July Effect where doctors have failed?
One cause could be the business researchers’ use of more comprehensive data. Whereas most studies look at hospitals in one region or a number of cases for a particular procedure, Huckman and co. draw on a national survey that provides 5 years of data for some 20% of hospitals.
In addition, the Harvard researchers drew on an additional data set that allowed them to look at how much a teaching hospital relied on residents and interns — and therefore experienced turnover each July. This seems to be an important distinction, as they found that “minor teaching hospitals,” or those with less than one full-time resident for every four hospital beds, did not exhibit the dreaded July Effect.
Some healthy skepticism is warranted given all the studies casting doubt on the existence of a July Effect, but the authors do offer additional evidence that lends credibility to the findings. They calculate the July Effect by comparing the performance of teaching hospitals and non teaching hospitals throughout the year, and they find that the gap between the two is greatest in July and August, lingers until December, and then is gone by January once the teaching hospital staffs have grown accustomed to their new roles. (So the July Effect actually lasts for half the year.) Further, the authors find the same pattern when looking at mortality rates and length of stay in the hospital for Medicaid recipients, who rely more on teaching hospital doctors.
What This Means
The work of Huckman and co. is a working paper, meaning that it has been released in non-final form to garner feedback and criticism. But even its current form does not offer clear conclusions. The authors estimate that the July Effect is associated with “roughly 1,500 to 2,750 accelerated deaths per year in the United States,” which is worrisome. But that is still only a fraction of a percent of the over 700,000 mortalities that occur in hospitals each year. And as indicated by the term “accelerated deaths,” the authors cannot conclude how many mortalities were patients that would have made full recoveries and how many were chronically ill patients that died several days earlier than they would have otherwise.
The premise of the July Effect is that the practice of having nearly all medical students and residents assume new responsibilities at the same time is particularly disruptive. But the authors also find evidence that teaching hospitals with the highest share of residents actually don’t exhibit the July Effect. When they split the major teaching hospitals into three tiers, the July Effect persisted for all but the tier with the greatest share of residents per patient — something the authors attributed to those hospitals having more supervisors. The authors’ theory comes from looking at hospital data on supervision, but it agrees with the observation of the aforementioned ob/gyn resident who writes, “I’d argue that the reason the [July Effect] is not seen is directly related to the counter-coup phenomenon of July: more hand-holding and more vigilance from above.”
The Harvard Business School academics chose to investigate the July Effect not because they did not trust doctors to get it right, but to inform the debate in the business world about turnover. It’s a diverse debate that often sees turnover as a negative force, leading to additional training costs and lost expertise; but it also can see churn as a positive development, depending on the industry and type of task at hand, that brings in fresh energy or new ideas. Looking at the July Effect is helpful because it avoids all the complicated questions about which type of employees tend to stay at typical companies and which tend to leave.
The findings lend ammunition to the idea that, generally speaking, turnover has negative effects. It is particularly applicable to other industries that have all-in-one-go turnover; just as patients may want to ask about the quality of care in July, companies hiring consulting firms may want to question the quality of the team they hire when new consultants join straight out of undergrad and business school.
But the paper also suggests that the most important factor is how companies or organizations prepare for turnover. Take the example of America’s diplomats in Iraq and Afghanistan. As both locations were classified “extreme hardship” posts, the foreign service only required that diplomats work there for one year. As a result, every summer, diplomats with a year’s worth of experience in the country cycled out and greenhorn replacements cycled in — often during critical junctions like Afghanistan’s most recent election. This author recalls a high ranking diplomat who served in the region complain about the policy, stating, “We’re at war, dammit.”
In contrast, the Harvard researchers’ findings suggest that teaching hospitals with the most residents also incorporate the most supervision, prepare for the transition, and ride it out without negative consequences. A July Effect may mainly be a problem in industries that are unaware of it or unwilling to step up and tackle the accompanying challenges. Doctors’ jokes about the July Effect may seem in poor taste given the potentially deadly consequences, but they have a positive side: Beware any industry too blithe or unaware to joke about the newbies messing everything up.
This post was written by Alex Mayyasi. Follow him on Twitter here or Google Plus. To get occasional notifications when we write blog posts, sign up for our email list.



